
Before you read this post, I recommend reading Nora’s Birth Story (and watching Nora’s Birth Video!) for more context.
First few days

I shared about my immediate postpartum experience in this post, so I won’t spend too much time on it here. In short, I birthed Nora, and due to a nuchal hand, suffered from a third degree tear. Although a third degree tear is a painful and significant birth injury, it’s not wholly uncommon; I assumed I’d have a relatively slow recovery, but that my recovery would be linear nonetheless. Unfortunately, I was wrong–but we’ll get to that later.

The first few days after Nora was born were a blur. I was mentally and physically exhausted while simultaneously feeling overwhelmed by love. I remember getting her dressed when she was two days old and sobbing out of the overflow of love and adoration I felt for her. She was so perfect and precious in every way.

One evening, I was holding Nora’s tiny sleeping body on my chest while watching TV in bed. I started to cry tears of joy. Riley walked in and asked what was wrong, to which I responded, “I think this is the happiest I’ve ever been!” Those first few days were truly precious.
November
Midwife home visit
When Nora was three days old, we had our first midwife home visit with Midwife Judith. It was wonderful to be able to stay in bed and have a care provider come to me! The visit lasted close to three hours and was incredibly thorough–both of our vitals were checked, Nora was weighed and measured again, the midwife helped us with breastfeeding, my tear and healing was inspected, we went over the birth, we talked about nutrition, etc.

It was determined that both of us were doing extremely well and that although it was early, I was beginning to heal correctly. There were two things to note: firstly, Nora had severe lip and tongue ties, which were responsible for our extreme difficulty with breastfeeding, and secondly, that Nora was slightly jaundiced.

A pediatric dentist was recommended to correct the ties and Judith recommended that I continue to nurse Nora on-demand and have Riley “sun” her in our car a few times a day to help with the jaundice. Following this protocol, her jaundice was gone within a couple of days.
Lip and tongue tie revision
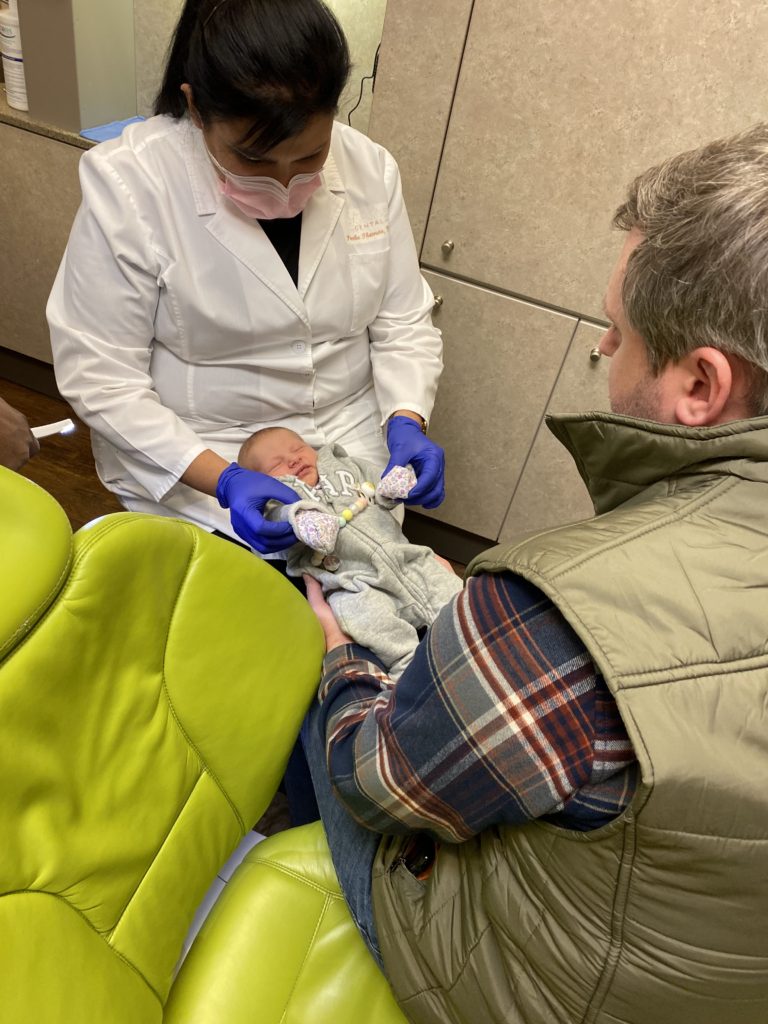
When Nora was only six days old, we went to a highly recommended pediatric dentist who specializes in lip and tongue tie revisions (she’s done over 5,000 of them!). Her office was about an hour away from our house, so we loaded up for our first family outing. (If you live in the DFW area, I highly recommend Enclave Dental for revisions.)

I was absolutely terrified. I remember asking Riley to take a photo of me and Nora (above) in the dentist’s waiting room to document our first outing. After he took it, he said jokingly “You look scared!” I responded, “I am scared!” The last thing I wanted to do at six days postpartum was drive an hour away for my newborn to have her mouth lasered.
That said, breastfeeding had become excruciating. It was so painful that it was almost impossible; in fact, for the 24 hours before her procedure, I was pumping and bottle feeding Nora because breastfeeding was so horrific.
I remember crying on the phone to one of my midwives before her procedure, “Nursing is way worse than childbirth!” Every time Nora would latch, I would grit my teeth and cry in agony. It was awful. My midwife Kaitlyn talked me down, explained the procedure from start to finish, and gave me peace of mind about proceeding. All that in mind, I knew getting her ties revised was the right path.
The procedure went perfectly and took literally 30 seconds, but it was emotional and difficult for me. Riley stayed with Nora while I stepped into the hallway and cried. I was only six days postpartum–still in significant pain and discomfort, hormones everywhere, feeling guilty that I couldn’t make breastfeeding work with Nora without this procedure, and a million other things. (For a quick snapshot of why tongue/lip tie revisions are sometimes necessary, check out this Instagram post–excuse the language; the photo is great though and exactly what Nora’s latch looked like before and after.)
After her procedure, my midwives invited me to drive to the birth center so that they could help me learn how to latch Nora properly, now that she was physically able to latch properly. I laid back in bed (in the room I gave birth in, actually!), and my midwife Roxanne lounged next to me and helped me. It was so helpful and I immediately felt a massive difference in breastfeeding.
As draining as it was, looking back, having this procedure was the single best decision we made for our breastfeeding relationship; it truly made all the difference.
The baby blues
Starting at day three or four postpartum, my birth high crashed and I began to feel “off.” This is natural and normal and referred to as “the baby blues,” and is attributed to the massive hormonal shifts that occur immediately after a woman has a baby. I knew it was normal to be weepy and overwhelmed, and both my midwives and doula were checking in with me daily or near-daily to monitor my emotional health.
D-MER diagnosis
Once the physical difficulty with breastfeeding was resolved, I began to notice a horrible, nauseous, depressing feeling sweep over me each time Nora nursed. I had been experiencing this for weeks, but I attributed it to her poor latch. With the latch corrected, it was more noticeable. I remember sitting at my two week follow-up appointment and telling Midwife Kaitlyn, “I really don’t enjoy nursing. It feels awful.”
She asked me a series of questions before concluding, “It sounds like you have D-MER, or dysmorphic milk ejection reflex. It’s a hormonal issue that makes you feel nauseous and sad each time your milk lets down.”
In that moment, I felt like Anne Hathaway’s character in The Princess Diaries. “As if I’m not enough of a freak already, let’s add a tiara!” As if I wasn’t dealing with enough already–a third degree tear, lip and tongue tie revisions, the baby blues, and everything else–let’s add a bizarre breastfeeding problem!
December
Symptoms of depression
Unfortunately, as the days and weeks progressed, my “baby blues” began to spiral downward. I started feeling absolutely terrible. I would weep all the time. Everything felt overwhelming, from taking a shower to making the bed to folding a basket of laundry. I was barely eating anything and I felt like I couldn’t get out of bed. Mind you, I was still physically healing and not getting very much sleep, but my symptoms were beyond those things.

I began to imagine horrible accidents happening. For example, I’d be carrying Nora into the kitchen to get a glass of water. I’d grab one and return to the couch or bed safely, and then I’d have these awful thoughts almost like flashbacks, where I’d imagine that when I walked into the kitchen, I hit Nora’s head on the doorframe or dropped her on the tile floor. These thoughts would happen constantly and were clearly extremely unsettling. I’d lay awake at night feeling overwhelmingly anxious about all the “what-ifs” during the day.
Emotional support appointment
Eventually, in early December, I realized that I needed help. A month had passed since Nora’s birth, and my emotional/mental health was deteriorating daily. I felt like I was drowning.
One afternoon, I called my mom. She could hear anxiety in my voice and immediately asked, “What’s wrong?” (How do moms just know?) I told her how I was feeling and she said, “I want you to hang up the phone and call Origins. Say, ‘I’m not doing well emotionally.’ See if you can get in for an appointment.” I was in such a bad headspace that I needed specific instructions like this; I hung up the phone and did exactly what she said.
A couple of days later, Nora and I went to Origins and met with Midwife Julie. She sat next to me on the couch and gently asked how I was doing, how I was feeling, how things were going, etc. I opened up and told her everything, including those terrible thoughts that I was having.
She was so kind. She put her hand on my shoulder and explained that I was experiencing intrusive thoughts, and that she suspected that I had a postpartum mood disorder.
While I was there, Julie also checked my healing. I was five weeks postpartum at this point and still in daily pain. She looked concerned and explained that my dissolvable stitches weren’t dissolving correctly and that she wanted me to meet with the OB/GYN that Origins works closely with, both to discuss the option of medication for my postpartum mood disorder and to determine what procedure(s) were necessary to get me back on the path to healing. She called and made an appointment for me with the doctor in a few more days.
OB/GYN appointment
This appointment was one of worst days of postpartum, and, to be honest, definitely in the bottom 10 percent of days of my life. I was in the worst mental state I’d ever experienced and had to get both myself and Nora ready, drive 90 minutes to the appointment in the heart of Dallas, navigate city traffic, figure out parking, and find an office I’d never been to before. On an average day, in an average state of mind, this is easy. On this day, in the state of mind I was in? Nearly impossible.
My appointment lasted over an hour. The doctor started by going over my mental health and diagnosed me with postpartum depression. She prescribed me an anti-depressant and instructed me to take a half-dose for two weeks and then increase to the full dose. I hadn’t been on an anti-depressant before, but I was hopeful that it would help me find my way out of the pit I was in.
After our mental health discussion, the doctor examined me. This was incredibly traumatic and painful. Come to find out, I’m in the very rare category of people whose bodies don’t break down suture material (likely due to being allergic to it), and as such, my stitches had barely dissolved at all in over five weeks. My tissue was healing/healed, but was essentially being pulled and pinched by undissolved stitches. No wonder I was in so much pain.
On top of that, internally, I had a four centimeter patch of granulation scar tissue. This was the main cause of my discomfort. After some discussion and more painful examination (all with Nora in her carrier beside the exam table), she explained that my situation required surgery to remove the granulation tissue since it would never get better or go away on its own.
I felt like someone had kicked me while I was down! The doctor handed me a tissue, but I held it together while I was in her office and scheduled the surgery for New Year’s Eve, right after getting home from holiday travel.
As soon as I got in the car with Nora, I began to sob. Like, hyperventilating, horrible, sobbing. I was so overwhelmed. I composed myself but decided not to call Riley and to wait to talk to him in person instead. I was afraid that calling him and relaying this information would be so upsetting that I wouldn’t be able to safely drive home–and all I wanted to do was go home. I dried my tears and started making my way home (during rush hour, I might add). Thankfully Nora slept peacefully in the back seat.
When I arrived home, Riley heard the garage open and came out to greet us. He told me he had a feeling that something was wrong even though we hadn’t spoken. He helped me and Nora inside, where he had a glass of wine and a big cheese board waiting for me. I recounted my appointment while he held Nora and I ate. Riley’s my rock; he always, always, always grounds me. This moment was no different. He reassured me that I’d be okay, even though it would be hard.
The next day, I texted my midwives’ on-call line to tell them that I required surgery. We went over the details of my situation before my Midwife Kaitlyn sent me this message:
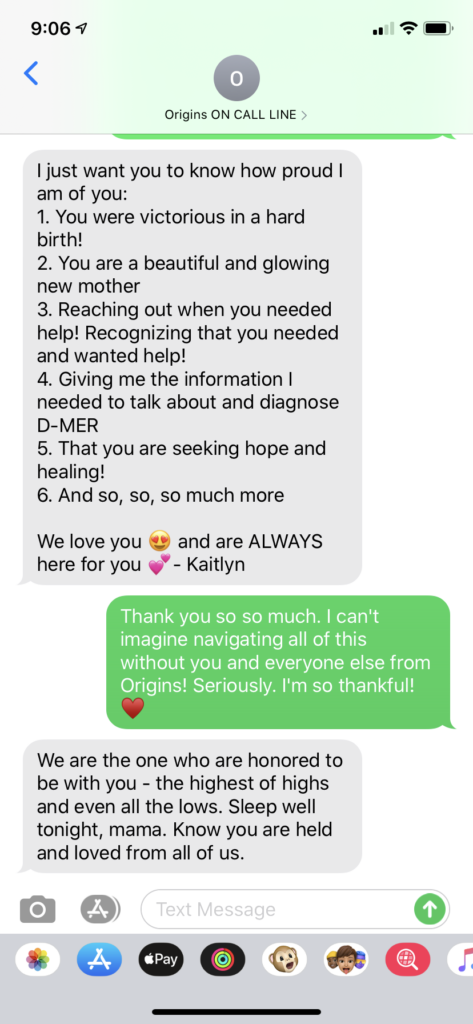
I honestly cannot imagine going through my postpartum experience (or pregnancy or birth) without the love and support of my midwives. They were/are incredible and their support has made all the difference.
Christmas in Maryland
We traveled to Maryland (my home state) for 10 days over Christmas. Both my midwives and doctor were hesitant to clear me to travel, but I really wanted to make the trip and basically begged them to let me go. I had been laying in bed for close to eight weeks straight and I desperately needed a change of scenery!

Being in Maryland was a mental break. Riley and I spent time together with and without Nora (her grandparents were happy to help!), we introduced her to her great-grandparents, celebrated Christmas and Riley’s birthday, and generally enjoyed being away.



Surgery on New Year’s Eve
My parents flew back with Riley, Nora, and me on December 30th in the afternoon so that they could help us while I recovered from surgery.
Surgery was on December 31st at 8am. We got up early to get ready, I got milk ready for Nora, and we drove into Dallas. I was so anxious that I was sick to my stomach. This was not only the first time I’d been away from Nora for more than an hour or so, it was also the first time I’d ever had surgery! (I did have my wisdom teeth removed a long time ago, but I hardly remember anything about it.)
We arrived and got checked in. In short, I kissed Riley goodbye, went back and got prepped, and met the anesthesiologist and my doctor. They explained what was going to happen and I was put under.
The next thing I knew, I was awake and it was all over. Thankfully, I didn’t feel confused, nauseous, or “out of it.” I was still numbed and feeling a bit sleepy, but otherwise, I felt normal. I was given instructions to take it easy and rest as much as possible, and to return for my follow-up the next week.
By the time we got home from surgery that day, I was extremely uncomfortable. For two or three days, I didn’t get out of bed at all. I nursed and cared for Nora the best I could, but I needed an extraordinary amount of help from Riley and my parents. I felt so helpless and frustrated.
January
Recovering from surgery
I’m so thankful for my parents’ help and Riley’s support because recovery was rough. I was in significant pain for a couple of weeks. The only thing my doctor could do for me was prescribe stronger pain medications, but I was uneasy about taking them given the fact that I was breastfeeding, so I stuck with ibuprofen.
Thankfully, the day of my surgery was about two weeks after I’d started my anti-depressant and I was really starting to feel back to myself mentally and emotionally. I knew my medication was working when both my mom and Riley independently commented how much lighter and more like myself I seemed (even though I was in pain). I can’t express what a massive relief it was for the intrusive thoughts to stop and to start feeling like I wasn’t completely drowning every single day. It felt like a thousand pounds had been taken off my shoulders.
With my mental health feeling better, my physical health slowly followed suit. Key word: slowly. I had four follow-up appointments following my surgery. At each one, my doctor/surgeon had to perform different procedures from burning off more scar tissue to cutting out stitches to injecting lidocaine, re-cutting a small incision, and re-stitching it. Horrific.
Unfortunately, I have some lingering trauma from all of these procedures, the surgery, and everything else I went through physically during the postpartum period. For close to four months straight, I was in around-the-clock pain. It clouded my mind and made me feel scared and nervous–I honestly wondered whether I’d ever feel normal again.
Each time I’d start to feel a little better, I’d have another appointment, more procedures, and would be back in pain. It really messed with my head and exhausted me. In some ways, I feel like my early days with Nora were stolen from me. I still haven’t processed it fully but will begin therapy to start to work on and heal the mental component in the next few weeks.
End of the “fourth trimester”
The end of January marked the end of my “fourth trimester,” or the end of the first three months postpartum. This was a strange milestone for me. On one hand, I was relieved to be “out of the woods,” starting to feel better, and well on my way to healing. On the other hand, my entire fourth trimester was underlined with pain. It was sometimes hard to soak up time with my precious newborn because of everything else going on.

February
Final post-op appointment
On February 18th, I had my last post-op appointment. My final stitches were removed (they’d been placed two weeks prior as a “revision” after surgery…) and I was finally, finally, finally done. What a relief.
After the mess of navigating the very first OB/GYN appointment alone, Riley took off work and accompanied me to every other one (except one, when my mom was in town and came with me). Bless that man.

I cried walking out the doctor’s office doors that day. I was absolutely overjoyed to be finished with seemingly endless procedures, each one more painful than the last. Finally. Finally, finally, finally.
Beginning to process early postpartum
In the days that followed, I experienced a range of emotions. Overwhelming relief and gratitude primarily, but also a feeling of deep sadness. For almost four months, I had been in terrible pain. Because of that pain, it had sometimes been difficult to soak up Nora’s newborn days. I felt like I was pretty much in pure survival mode every minute of every day with very few exceptions.
Celebrating with a girls’ trip

A few days after my final appointment, Nora and I flew to Maryland to spend a week in my hometown. I felt like I’d been stuck at home in bed forever and I was ready for a little adventure.
We had an amazing trip. We saw lots of my family members and friends, spent time with Nora’s little cousin Henry, and even met up with my sweet college friend, Angela.
My time in Baltimore was like a reset. In some ways, my time away felt like the bridge between all of the chaos and difficulty of my early postpartum experience and the healing and redemption that was beginning to flood our lives. Nora and I had so much fun!
Final thoughts on my postpartum experience
Now, at nearly five months postpartum, I’m able to look back with clearer eyes on my experience. For every part of my postpartum journey that brings me grief, anger, sadness, and trauma, there’s a part that brings me delight, joy, peace, and healing. I first learned what I was made of when I gave birth–that lesson continued through postpartum. Additionally, I learned how to ask for help, which has deepened my relationships profoundly.

I think this verse describes my experience beautifully: “You intended to harm me, but God intended it for good to accomplish what is now being done, the saving of many lives.” (Genesis 50:20, NIV)
The hell I walked through during my postpartum experience is nothing in comparison to what God is doing and will continue do with my story. I have the privilege of bearing a message of strength, hope, and healing amidst extreme brokenness.
What God has done for me, He can do for you.
I close this chapter with both a sigh of relief and a heart full of gratitude. I’ll never forget these days; these raw, thin, new days of becoming a mother.
Thank you for reading! You can find me online on YouTube, Facebook, Instagram, Pinterest, and Twitter. If you’d like to be alerted whenever I publish a new post, you can follow me on Bloglovin’ or subscribe via email. Check out my fun tees in my Etsy shop! Are you a blogger too? Check out my Blogger Mentorship Program.








Oh Blair, I am so sorry that you experienced all that you did. Even though your experiences are very different than mine, I can so understand that feeling of despair, and deep sadness when I look past on the fourth trimester after I had my son. I just want to let you know you’re not alone and that it is so encouraging to hear that I’m not alone either. I think it is truly amazing how you were not afraid to ask for help and it is honestly inspiring. Thank you for sharing your story!
Thanks for reading, Ashley. Sending love!
Oh Blair! Thank you for being so vulnerable in sharing your story. During my conceiving journey (which was much like yours- over a year) I went through an extreme period of anxiety and depression filled with intrusive thoughts. I thought I was crazy and a terrible person. Reaching out, bringing it to the light, and sharing was the hardest thing to do but WOW! The redemption the Lord brings. So proud of you and thankful you are recovering. Praying for you, Riley, and Nora in the coming days. For joy and peace to be abounding. 🙂
Thank you for reading and for your sweet comment, Meredith!
Thank you for being so candid and honest about the realities of life after giving birth, especially the mental/emotional aspect. I know from personal experience that it is helpful to hear stories of other women going through the same experience as you are. Having children really helps you discover strength that you didn’t know you had.
“A woman is like a tea bag. You can’t tell how strong she is until you put her in hot water.”
~ Eleanor Roosevelt
Great quote, and so true. Thanks for reading, Angela!
This is so beautiful and honest. I so appreciate you talking about intrusive thoughts. It can be difficult to admit and feel so conflicting when you are overwhelmed by love and fear at the same time. Also thank you for your honesty about meds – there is so much stigma to taking these as a new mom! If you are still taking them, how did you manage with your ‘crunchy’ leanings?
I have a couple questions!
What did you do to deal with the DMER? Did the meds help with this? Did breastfeeding get easier if you still are? I just had to stop breastfeeding and there is so much guilt associated with it.
Would you ever see an OB again if you needed to, or would you seek somewhere else? It sounds like your experience was really negative, but not sure if this was the doctor or just the horrible situation.
Hi Janet!
Yes, I’m still on meds. They’ve made a huge difference. I’ll go off them when I’m ready, but I’m not there yet.
For all intents and purposes, there’s no cure for DMER. The meds don’t touch it. I’ve learned that when I’m dehydrated or very sleepy, it’s worse. But it hasn’t gone away. I’ve learned to breathe through it and wait for it to pass during each breastfeeding session.
I really respected and appreciated my OB. She was fantastic. It was my situation that was horrible. My birth center offers yearly exams (exactly like what an OB/GYN offers), so I’ll likely do that, but if I need to go to an OB in the future, I’ll go to the one who helped me through postpartum.
Hope that helps. Thanks for reading!
Hi Blair,
I’ve been reading your blog for years now (through high school, college, and now my first job!), and I was so grateful to see a new post today! Thank you for providing something to read other than COVID news, and for being so encouraging. Thank you for being so vulnerable and open. Thank you for always pointing your readers back to the Lord! Thank you for being an advocate for mental health and therapy (advice that I have recently taken). And thank you for letting us internet strangers be a part of your life. It’s great to hear that you and Nora are still doing well.
<3 Lily
Blair, you really weathered an intense storm— actually multiple intense storms! Thank you for sharing and helping other moms not to feel alone. I struggled with breastfeeding for different reasons, but it is very validating to know I wasn’t alone in my struggle and that breastfeeding is HARD.
I don’t know if this will help you or not, but I really identified with what you said about those newborn days feeling stolen from you. I think the new mom adjustment is such a whirlwind no matter what the postpartum experience that we all feel this way. I hope this doesn’t sound like I am minimizing your very traumatic experience. What I mean to say is, like the poignant new mom quotes you’ve posted, is that even without having an especially difficult 4th trimester, I look back on that time and feel like I was in complete shock, just going through the motions. I wish I could have a do-over, too.
Hey Blair. Thanks for sharing.
All of us have different pregnancies and postpartum experiences. Though mine was very different to yours, it is so amazing to see you share your story.
You are a light for so many, especially during these times of isolation. One of my friends said “I’m just thankful for the fact that Jesus is in control and we can look to him for comfort and provision” and it is so true.
God bless x
This is just beautiful, and made me cry! So many of the things you mentioned- postpartum depression, DMER, painful breastfeeding- happened to me as well, although nearly 10 years ago now! Unfortunately, I didn’t ask for help and just weathered the storm on my own. I can’t help but wonder how much better those early days could have been if I had help, and that makes me so sad. I’ll never know, but I hope that this message reaches women going through the same things and encourages them to ask for help! Sending you love and prayers for continued healing.
Oh my gosh, my heart hurt for you! I’m so grateful that you are finally on the road to recovery, and hope your sweet little family is weathering this latest Covid-19 wrinkle with the same grace that has carried you through all that came before! Thank you for sharing your story!
I’m so glad you shared this story. It’s going to help so many other women who may feel alone in their postpartum journey. I’m also SO glad you’re doing better! Trauma with pregnancy and birth takes a while to recover from and people rarely talk about it. It took me two years after Zoey was released from NICU to not be terrified, to feel like I could do it again, and for the nightmares to stop. Praying that your continued recovery gets better and better!
Oh Blair. I am so sorry you had such a difficult recovery. That sounds so hard. I am so grateful though that you are sharing your story. You have always been so good at being real and genuine in this space. I am so grateful and hope you are feeling better. You are in my prayers and I hope you are enjoying this time with precious Nora.